Bloating, brain fog, skin flares, and fatigue that never fully resolves — these are among the most common complaints I hear in practice. And in many cases, what connects them is a gut barrier that is no longer doing its job.
Intestinal permeability — commonly called "leaky gut" — is a condition in which the lining of the small intestine becomes compromised, allowing partially digested food particles, bacterial fragments, and other substances to pass into the bloodstream. What follows is a cascade of immune activation and systemic inflammation that can drive symptoms in virtually every system of the body.
The frustrating reality is that leaky gut rarely shows up on standard lab work. It is not a diagnosis that most conventional providers are trained to look for, and its symptoms are so varied and diffuse that they are often attributed to stress, aging, or simply "just how you are." Understanding what leaky gut actually is — and how to identify it — is the first step toward addressing it.
What Is Intestinal Permeability?
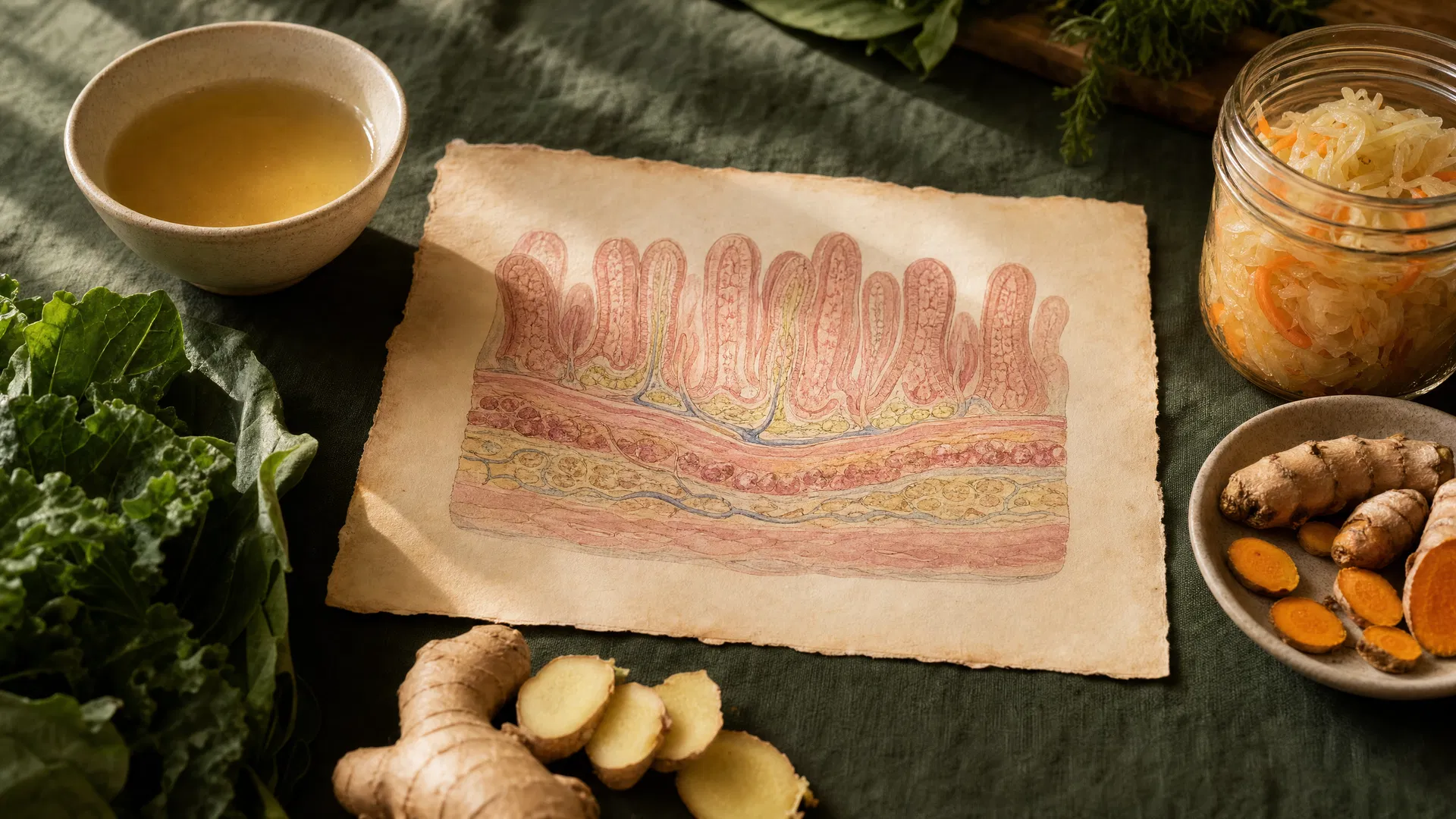
The lining of the small intestine is a remarkable structure. It is only one cell layer thick — a single row of epithelial cells connected by tight junction proteins that act like gatekeepers, selectively allowing nutrients to pass through while keeping harmful substances out. When functioning properly, this barrier absorbs what the body needs and excludes what it does not.
When the tight junctions become damaged or loosened — by chronic stress, processed food, alcohol, medications like NSAIDs and antibiotics, infections, or dysbiosis (imbalanced gut bacteria) — the barrier becomes permeable. Substances that should remain in the gut lumen begin slipping through the gaps into the bloodstream.
The immune system, which lines approximately 70 percent of the gut wall, responds to these foreign particles as threats. It mounts an inflammatory response — and because the bloodstream carries these particles throughout the body, the inflammation is systemic. This is why leaky gut can manifest as symptoms in the brain, skin, joints, sinuses, and hormonal systems, not just the digestive tract.
It is worth noting that intestinal permeability exists on a spectrum. Some degree of increased permeability can occur temporarily with illness, intense exercise, or dietary changes. The concern arises when it becomes chronic and persistent, creating a continuous cycle of immune activation that the body cannot resolve on its own.
Common Signs and Symptoms
Because leaky gut drives systemic inflammation rather than a single localized reaction, its symptoms are wide-ranging. No single symptom confirms intestinal permeability — but a cluster of the following, particularly when they have been present for months or years without a clear explanation, warrants a closer look.
Digestive symptoms are often the most obvious: chronic bloating, gas, and distension that worsens after meals; alternating constipation and loose stools; abdominal discomfort or cramping; and a general sense of digestive unpredictability. Many people with leaky gut have been told they have IBS — and while that label may be accurate, it does not explain why the IBS developed or what is driving it.
Beyond the gut, the signs are frequently surprising to those who have never connected their symptoms to digestive health. Skin conditions — particularly eczema, psoriasis, rosacea, and adult acne — are among the most common extra-intestinal manifestations of gut barrier dysfunction. The skin and the gut share embryological origins and are deeply connected through immune pathways; when the gut is inflamed, the skin often reflects it.
Neurological and cognitive symptoms are equally common. Brain fog — the persistent sense of mental cloudiness, slow processing, and difficulty concentrating — is one of the most frequently reported complaints in clients with leaky gut. Anxiety, mood instability, and low stress resilience are also closely associated, as the gut-brain axis is profoundly sensitive to intestinal inflammation. Headaches and migraines that have resisted conventional treatment may also have a gut component.
Joint pain and stiffness, chronic fatigue that is disproportionate to activity level, frequent illness or slow recovery from infections, and hormonal irregularities — including thyroid dysfunction and cycle-related symptoms — round out the picture. Autoimmune conditions in particular have a well-established connection to intestinal permeability; the research suggests that leaky gut may be a necessary precondition for autoimmunity to develop in genetically susceptible individuals.

What Causes the Gut Barrier to Break Down?
Intestinal permeability does not develop overnight. It is typically the result of multiple overlapping stressors accumulating over time. Understanding the drivers is essential, because healing the barrier requires addressing the causes — not just patching the symptoms.
Diet is one of the most significant contributors. Highly processed foods, refined sugars, industrial seed oils, and food additives (particularly emulsifiers and artificial sweeteners) have been shown to disrupt the gut microbiome and compromise tight junction integrity. Gluten — specifically the protein gliadin — directly stimulates the release of zonulin, a protein that loosens tight junctions. This does not mean everyone needs to avoid gluten permanently, but in the context of an already-compromised barrier, it can perpetuate the cycle.
Chronic stress is equally damaging. The stress response triggers the release of cortisol and other hormones that directly affect gut motility, microbiome composition, and barrier integrity. People under prolonged psychological or physiological stress — including overtraining, sleep deprivation, and emotional strain — consistently show markers of increased intestinal permeability.
Medications, particularly non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and naproxen, are well-documented disruptors of the gut lining. Antibiotics, while sometimes necessary, alter the microbiome in ways that can take months to recover from and may leave the barrier vulnerable. Proton pump inhibitors (PPIs), used for acid reflux, alter the gut environment in ways that promote dysbiosis.
Gut infections and dysbiosis — overgrowths of opportunistic bacteria, parasites, or fungi — create a pro-inflammatory environment that both damages the barrier and prevents it from healing. This is why addressing leaky gut often requires a comprehensive stool analysis alongside barrier testing, to identify what is living in the gut and contributing to the problem.
How Is Leaky Gut Tested?
This is where functional testing becomes invaluable — because standard blood work does not measure intestinal permeability. A normal CBC, metabolic panel, or even a standard GI workup will not reveal a compromised gut barrier. This is one of the primary reasons leaky gut goes unidentified for years in so many people.
The Advanced Intestinal Barrier Assessment (AIBA) from Precision Point Diagnostics is one of the most comprehensive tools available for evaluating gut barrier function. Rather than relying on a single marker, the AIBA uses a panel of innovative biomarkers to assess multiple aspects of barrier integrity simultaneously.
The test measures Occludin and Zonulin antibodies — proteins that are directly involved in tight junction structure. When the barrier is compromised, these proteins are exposed to the immune system, which produces antibodies against them. Elevated antibodies indicate that the barrier has been breached and the immune system has been activated. The AIBA also measures Lipopolysaccharide (LPS) antibodies — LPS is a bacterial endotoxin that should remain in the gut but leaks into the bloodstream when permeability is present, triggering a significant inflammatory response.
Together, these markers provide a detailed picture of whether intestinal permeability is present, how significant it is, and which aspects of the barrier are most affected. This information directly guides the healing protocol that follows.
The AIBA is most powerful when paired with a GI Map stool analysis, which evaluates the microbial environment of the gut — identifying pathogens, dysbiosis, inflammation markers, and digestive function. Knowing both what is happening to the barrier and what is living in the gut allows for a truly targeted and comprehensive approach.
It is also worth noting that Zonulin can be added as an individual marker to the GI Map panel. Zonulin is a protein that directly regulates the opening and closing of tight junctions in the intestinal lining. Elevated stool zonulin levels are a meaningful indicator of active barrier disruption and can provide an additional layer of confirmation when intestinal permeability is suspected, particularly for clients who want a comprehensive picture before committing to the full AIBA panel.

What Does a Gut Healing Protocol Look Like?
Healing intestinal permeability is not a single intervention — it is a structured, multi-phase process that addresses the root causes, repairs the barrier, and restores a healthy microbial environment. The specific protocol is always individualized based on test results, health history, and contributing factors, but the general framework follows a logical sequence.
The first priority is removing the drivers. This means identifying and eliminating the dietary triggers, stressors, and microbial imbalances that are perpetuating the damage. For some clients, this involves removing highly reactive foods identified through MRT testing. For others, it means addressing a specific pathogen or overgrowth identified on the GI Map. Reducing NSAID use, supporting stress physiology, and improving sleep are equally important at this stage.
Repairing the gut lining comes next. Several nutrients have strong evidence for supporting tight junction integrity and epithelial repair. L-glutamine is the primary fuel source for intestinal epithelial cells and is one of the most well-researched gut-healing nutrients. Zinc carnosine has been shown to stabilize the gut lining and reduce intestinal inflammation. Deglycyrrhizinated licorice (DGL), slippery elm, and aloe vera support the mucosal layer that protects the epithelium. Specific peptides may also be used to support tissue repair.
Restoring the microbiome is the third pillar. A healthy, diverse gut microbiome is essential for maintaining barrier integrity — beneficial bacteria produce short-chain fatty acids like butyrate that directly nourish the gut lining and regulate tight junction expression.
Dietary fiber is one of the most powerful tools for microbiome restoration, and variety matters as much as quantity. Different types of fiber feed different bacterial populations. Soluble fibers — found in oats, legumes, apples, and psyllium — form a gel in the gut and are fermented by bacteria into butyrate and other short-chain fatty acids. Insoluble fibers — found in vegetables, whole grains, and seeds — add bulk and support motility. Resistant starch — found in cooked and cooled potatoes, green bananas, and legumes — is particularly effective at feeding butyrate-producing bacteria. Prebiotic fibers such as inulin and fructooligosaccharides (FOS), found in garlic, onions, leeks, asparagus, and chicory root, selectively nourish beneficial Bifidobacterium and Lactobacillus species.
Fermented foods provide living microorganisms that can help repopulate and diversify the gut ecosystem. Yogurt with live active cultures, kefir, sauerkraut, kimchi, miso, tempeh, and kombucha all contribute different strains and metabolites. Introducing these foods gradually is important, as some individuals with significant dysbiosis may initially react to fermented foods and need to build tolerance slowly.
Postbiotics — the bioactive compounds produced by bacteria during fermentation — are an emerging and important area of gut health support. These include short-chain fatty acids (particularly butyrate), bacteriocins, enzymes, and cell wall fragments that exert direct anti-inflammatory and barrier-protective effects. Supplemental butyrate, in the form of sodium or calcium butyrate, can be particularly useful when dietary fiber alone is insufficient to restore adequate levels, or during the early phases of healing when the microbiome is still rebuilding.
Reducing systemic inflammation supports the healing process throughout. Anti-inflammatory dietary strategies and omega-3 fatty acids from fatty fish, flaxseed, and high-quality fish oil help quiet the immune response while the barrier rebuilds. Specific botanicals — including curcumin (from turmeric), quercetin, and boswellia — have well-documented anti-inflammatory and gut-protective properties and are commonly incorporated into gut healing protocols.
Specific peptides play an increasingly recognized role in both gut healing and systemic inflammation reduction. BPC-157 (Body Protection Compound) is a peptide derived from a protein found in gastric juice that has shown remarkable tissue-healing properties in research, including the ability to accelerate repair of the intestinal lining, reduce gut inflammation, and support angiogenesis (new blood vessel formation) in damaged tissue. Larazotide acetate is a peptide that directly targets and stabilizes tight junction proteins, helping to prevent further permeability while healing is underway. These peptides represent a more targeted layer of support that may be considered in cases of significant or longstanding barrier dysfunction.
This is not a quick process — meaningful gut healing typically takes anywhere from four to eighteen months depending on the severity of the barrier dysfunction, the underlying drivers, and how consistently the protocol is followed. The timeline varies significantly from person to person, but the results, when the protocol is properly matched to the individual, are often transformative.

When to Seek Functional Support
If you have been dealing with chronic digestive symptoms, unexplained skin conditions, persistent brain fog, fatigue, or mood instability — and conventional approaches have not provided satisfying answers — intestinal permeability may be a significant piece of your picture.
The most important thing to understand is that leaky gut is not a life sentence. It is a functional condition that developed in response to identifiable stressors, and it can be meaningfully improved when those stressors are addressed and the barrier is given the support it needs to heal.
Working with a practitioner who understands both the testing and the clinical application of gut healing protocols makes a significant difference. The goal is not to follow a generic "gut health" program, but to understand your specific barrier status, your individual microbial environment, and the particular drivers that have contributed to your situation — and to build a protocol that addresses all of them in a logical, supported sequence.
If you are curious whether intestinal permeability may be contributing to your symptoms, a free 15-minute discovery call is a good place to start. We can discuss your health history, what testing might be most relevant, and what a personalized approach could look like for you.
Clinical Note
"The AIBA and GI Map are the most powerful combination for understanding gut barrier dysfunction — one tells you the state of the barrier, the other tells you what is living in the environment driving it."
— Julia Callaghan, CLT
Found this helpful? Share it with someone who might need it.

Written by
Julia Callaghan, CLT
Julia is a Functional Nutritionist and Certified Leap Therapist (CLT) based in Charlotte, NC, serving clients throughout Charlotte, Waxhaw, and the greater Charlotte metro area. She holds a B.S. in Human Nutrition from Winthrop University (cum laude) and has completed the Applying Functional Medicine in Clinical Practice (AFMCP) program with the Institute of Functional Medicine. Her practice focuses on identifying and addressing the root causes of chronic symptoms through functional lab testing and personalized nutrition protocols.
Wondering if Leaky Gut Is Part of Your Picture?
A free 15-minute discovery call is a good place to start. We can review your symptoms, discuss which testing may be most relevant, and explore what a personalized gut healing protocol could look like for you.